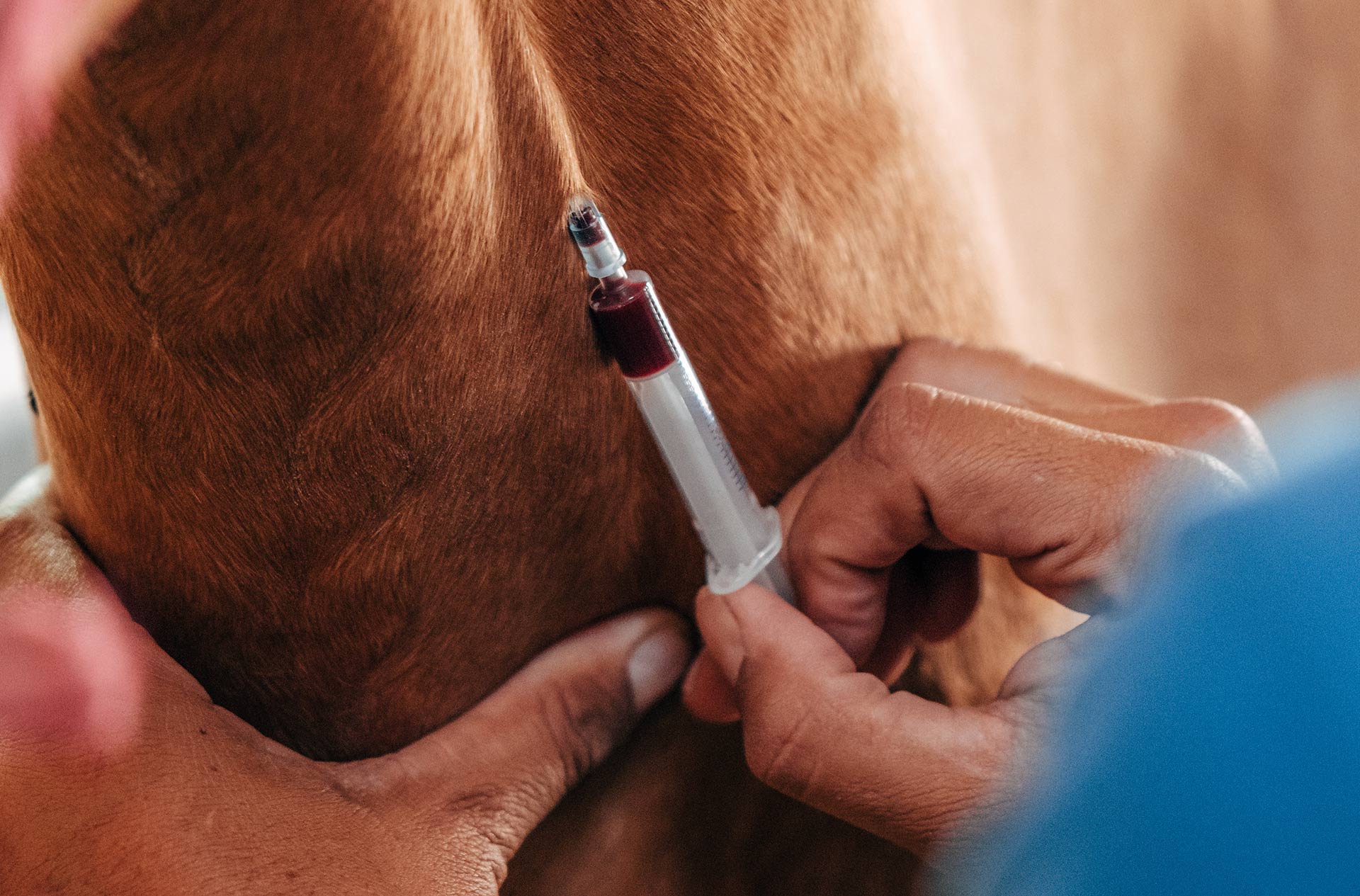
Six-panel genetic testing for horses is a diagnostic tool used by horse owners, breeders, and veterinarians to assess the genetic predisposition of a horse to specific hereditary diseases or traits. This type of testing provides valuable information about a horse’s genetic makeup, allowing for informed breeding decisions and proactive management of potential health concerns. Here’s an explanation of what a six-panel genetic test typically includes: Hereditary Equine Regional Dermal Asthenia...